- Blog
- Integrin Activation Pmanet
- Download Makalah Psikologi Pendidikan Pdf To Jpg
- Cyberpunk 2020 Protect And Serve Pdf To Word
- Download Undangan Pernikahan Dengan Word Finder
- Game Manual Madden 07 Game Boy Advance Rom
- Serial Communication With Gsm Modem Sim 800 H
- Dream Team Fsx Crack Code
- Update Row In Datatable Using Linq Distinct Query
- Esonic Driver For Win7
- Alice Munro Dance Of The Happy Shades Pdfescape
- Cam 350 Software Crack Downloads
- Khatrimaza Flash Movie
- All Star Yakyuken Battle Psp Go Hack
- Numento Keygen Mac Torrent
- Download Iis PS1 Gekisou Tomarunner
- Download Camtasia Studio 7 Full Crack 32 Bit
- Game Who Wants To Be A Millionaire Online Versi Indonesia
- Thillalangadi Movie 5.1 Dvd Untouched
- Race 2 Bluray Torrent
- How To Crack A Tripcode Decoder Glasses
- Consuming Fire Tim Hughes Pdf Converter
- Baca Novel Terjemahan Linda Howard
- Edi 1300 Keygens
- Logon Screen Windows 7 Anime Skins
- Gratis Style Dangdut Yamaha Psr S700 Eladó
- Diploma Mechanical Engineering Book In Tamil
- Skype Voip Phone Driver
- Creating rhinestone templates in inkscape
- Telecharger god of war 3 ps2 iso
- Netcat windows download win7 32
- Uninstall metropolis ark 1
- The promised neverland manga 84
- 3-5 character sheet interactive
- Vip fortnite cheats legit
- Nba 2k14 update rosters
- Vietnamese fonts for word
- Floor plan vr how to get cowboy arm
- Omnisphere vst zip
- Sothink video converter failed to add the following files
- Download browsec premium
- Wii u emulator
- Aiptek tablet application
Integrin-mediated signalling through the MAP-kinase pathway Abstract The mitogen activated protein (MAP) kinase cascade, leading to extracellular-regulated kinase (ERK) activation, is a key regulator of cell growth and proliferation. The effects of ERK are mediated by differences in ERK signalling dynamics, including magnitude and duration.
Abstract Retinal pigment epithelial cell malfunction is a causative feature of age-related macular degeneration, and transplantation of new retinal pigment epithelial cells is an attractive strategy to prevent further progression and visual loss. However, transplants have shown limited efficacy, mainly because transplanted cells fail to adhere and migrate onto pathological Bruch’s membrane. Adhesion to Bruch’s membrane is integrin-mediated. Ageing of Bruch’s membrane leads to a decline in integrin ligands and, added to this, wet age-related macular degeneration leads to upregulation of anti-adhesive molecules such as tenascin-C. We have therefore investigated whether manipulation of integrin function in retinal pigment epithelial cells can restore their adhesion and migration on wet age-related macular degeneration-damaged Bruch’s membrane.
Using spontaneously immortalized human retinal pigment epithelial cells (adult retinal pigment epithelium-19), we show that adhesion and migration on the Bruch’s membrane components is integrin-dependent and enhanced by integrin-activating agents manganese and TS2/16. These allowed cells to adhere and migrate on low concentrations of ligand, as would be found in aged Bruch’s membrane. We next developed a method for stripping cells from Bruch’s membrane so that adhesion and migration assays can be performed on its surface. Integrin activation had a moderate effect on enhancing retinal pigmented epithelial cell adhesion and migration on normal human and rat Bruch’s membrane. However, on Bruch’s membrane prepared from human wet age-related macular degeneration-affected eyes, adhesion was lower and integrin activation had a much greater effect.
A candidate molecule for preventing retinal pigmented epithelial interaction with age-related macular degeneration-affected Bruch’s membrane is tenascin-C which we confirm is present at high levels in wet age-related macular degeneration membrane. We show that tenascin-C is anti-adhesive for retinal pigmented epithelial cells, but after integrin activation, they can adhere and migrate on it using alphaVbeta3 integrin. Alternatively, we find that transduction of retinal pigmented epithelial cells with alpha9 integrin, a tenascin-C-binding integrin, led to a large increase in alpha9beta1-mediated adhesion and migration on tenascin-C. Both expression of alpha9 integrin and integrin activation greatly enhanced the ability of retinal pigment epithelial cells to adhere to tenascin-rich wet age-related macular degeneration-affected Bruch’s membranes. Our results suggest that manipulation of retinal pigment epithelial cell integrins through integrin activating strategies, or expression of new integrins such as alpha9, could be effective in improving the efficacy of retinal pigment epithelial cell transplantation in wet age-related macular degeneration-affected eyes. , Introduction Age-related macular degeneration is the leading cause of blindness in the developed world (Jager et al., ). Advanced age-related macular degeneration is characterized by focal deposits of amorphous material known as drusen, formation of choroidal new vessels, photoreceptor loss, retinal detachment, subretinal haemorrhage and visual loss (Fine et al., ).
At least some of these changes can be ascribed to age-related malfunction of the retinal pigmented epithelium (RPE) and the underlying Bruch’s membrane. The RPE has multiple roles in the metabolic support of the retina and in phagocytosis of shed photoreceptor outer segment fragments.
Current treatment of wet age-related macular degeneration aims to halt the retinal damage due to neovascularisation. It includes removal of choroidal new vessels using techniques such as photodynamic therapy and photocoagulation (Gehrs et al., ). Replacement of the RPE is an attractive therapeutic option.
In animal models of age-related macular degeneration, RPE transplantation has been shown to be effective in preventing progressive photoreceptor and visual loss (Li and Turner,; Castillo et al., ). This has led to several trials of RPE replacement in human patients (summarized in Del Priore et al.,; Binder et al.,; da Cruz et al., ) with transplantation of dissociated RPE cells or grafts of RPE attached to the underlying choroid. Partial success has been obtained in some trials, and more recently a combined strategy of removing the pathological choroidal new vessels followed by transplantation of RPE cells has been tried (Algvere et al.,; Binder et al.,; MacLaren et al., ).
Where it has been possible to examine the fate of transplanted RPE cells, they have formed small aggregates, not attached to Bruch’s membrane and are therefore not positioned for maximal effect. Lack of adhesion of RPE cells to Bruch’s membrane is also detrimental to the survival of transplanted cells which undergo apoptosis if not attached to a surface (Tezel and Del Priore, ). Poor adhesion of RPE to Bruch’s membrane may also limit the migration of cells to achieve the repopulation of the denuded Bruch’s membrane exposed by surgery. For these reasons, transplants of patches of RPE attached to choroid or attached to a carrier substrate are probably the most promising current strategy (da Cruz et al., ).
There are several factors that affect RPE interactions with Bruch’s membrane. Ageing changes the membrane such that RPE cell adhesion is reduced (Del Priore and Tezel, 1999), and age also changes the pattern of gene expression and affects the capacity of RPE cells to phagocytose shed photoreceptor segments (Finnemann and Silverstein,; Cai and Del Priore, ). In age-related macular degeneration, Bruch’s membrane undergoes multiple pathological changes due to inflammation, scarring, aberrant extracellular matrix production and neovascularization, also rendering it unable to support RPE cell adhesion (Zarbin, ). In addition to these pathological changes, treatments to remove choroidal new vessels may damage or remove the superficial basal lamina of Bruch’s membrane, exposing the underlying layers, which are less adhesive to RPE cells (Grossniklaus et al.,; Tezel et al.,; Tsukahara et al., ). Various changes in the age-related macular degeneration-affected Bruch’s membrane affect its ability to support RPE cells, but of particular significance may be the upregulation of tenascin-C (TN-C). TN-C is an extracellular matrix glycoprotein that is anti-adhesive to many cell types, and which is upregulated in the damaged nervous system (Wehrle-Haller and Chiquet,; Kiernan et al.,; Scholze et al.,; Zhang et al.,; Tang et al., ). In wet age-related macular degeneration, TN-C expression is increased in regions of angiogenesis and neovascularization, and it is deposited in Bruch’s membrane on the basal side of RPE cells (Zagzag et al.,; Zagzag and Capo,; Fasler-Kan et al., ).
In addition very high levels of TN-C have been detected in neovascularized membranes removed from wet age-related macular degeneration patients (Nicolo et al., ). TN-C is therefore a candidate for causing the failure of RPE adhesion in damaged and aged Bruch’s membrane.
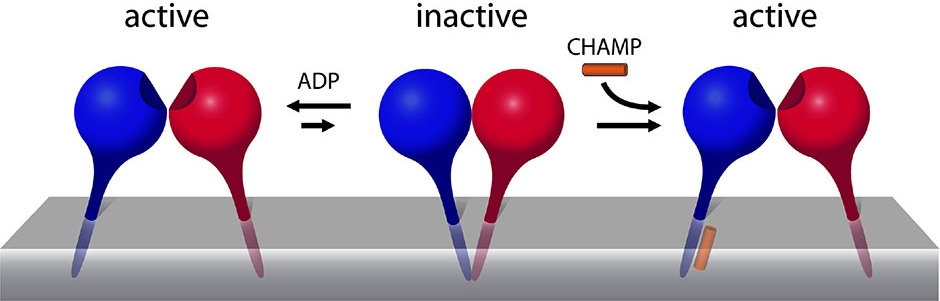
Attachment of cells to extracellular matrix structures is largely mediated via integrins, so manipulation of RPE integrins is a potential method for improving their adhesion and migration. Recent experiments in which integrins were manipulated before RPE transplantation support this idea. Prolonged culture of RPE cells, which leads to increased expression of integrin subunits (Zarbin,; Gullapalli et al., ) or genetic modification of RPE cells to overexpress alpha6beta4 integrin (Fang et al., ) both led to increased adhesion of RPE cells to various layers of Bruch’s membrane. Apart from altered expression, integrin function can be modulated by modifying the activation state, taking them from a low affinity inactive state to a high affinity active state favouring ligand binding and downstream signalling (Humphries, ). Forced integrin activation has been shown to enhance cell adhesion and migration and axon growth under non-permissive conditions such as low ligand availability or the presence of inhibitory molecules (Ivins et al.,; Miao et al.,; Hu and Strittmatter, ). In this study, we have asked whether various integrin-related interventions might enhance RPE cell adhesion and migration on normal and age-related macular degeneration-modified Bruch’s membrane and its components.
We show that integrin activation increases RPE attachment and migration on the extracellular matrix molecules that constitute Bruch’s membrane; then, using a new Bruch’s membrane preparation, we confirm these findings on normal adult membranes. Having confirmed that TN-C is greatly upregulated in pathological human Bruch’s membrane from wet age-related macular degeneration patients, we show that RPE attachment and migration is inhibited by TN-C, but that this inhibition can be overcome by integrin activation or expression of the tenascin-binding integrin alpha9. Finally, we show that these manipulations can allow RPE cells to interact with age-related macular degeneration-affected Bruch’s membrane.
Materials and methods Cell culture Adult retinal pigmented epithelium-19 (ARPE-19) RPE cell line was purchased from American Type Culture Collection (ATCC-HB243). Cells were cultured in RPE medium containing Dulbecco's; Modified Eagle’s Medium: F12; 1:1 ratio (ATCC), supplemented with 10% foetal calf serum (Invitrogen), and penicillin–streptomycin–fungizone (Sigma, 1%). RPE cells were cultured on poly- d-lysine (Sigma; 20 µg/ml) coated flasks. Viral preparation and transduction For preparing third generation, self-inactivating lentiviral vectors containing either farnesylated (f) green fluorescent protein (GFP) or α9-integrin-internal ribosome entry site-fGFP under control of the cytomegalovirus (CMV) promoter, plasmids were generously provided by Dr L. Naldini (University of Torino).
Lentiviral vectors were prepared as described in Andrews et al. Briefly, human embryonic kidney-293T cells were co-transfected using a calcium phosphate method to introduce two helper plasmids (pCMVdR84, containing lentiviral structural genes and pMD2.VSVG for pseudotyping) and the transfer plasmid (pRRLsin.PPT.CMV.fGFP.Wpre or pRRLsin.PPT.CMV.α-9-integrin-internal ribosome entry site-fGFP.Wpre, containing besides the transgenes, the HIV-1 cis-acting sequences, an expression cassette for the transgene driven by the CMV promoter, and the Woodchuck post-transcriptional regulatory element, Wpre). Following transfection, high titres of replication defective, self-inactivating vectors were released into the medium. The day after transfection, Iscove’s Modified Eagle Medium, supplemented with 10% fetal bovine serum and 50 µg/ml gentamicin (Gibco) was replaced. Medium was collected 48 h post-transfection and subjected to ultracentrifugation using an SW-28 rotor at 20 000 rpm. The transparent (yet yellowish-opaque appearing) pellet was resuspended in 500 μl phosphate buffered saline (pH 7.4), aliquoted and kept at −80°C until further use. Titration of the lentiviral vectors was performed using an enzyme-linked immunosorbent assay, directed against the p24 core protein (Perkin Elmer) according to the manufacturer’s protocol.
For transduction, RPE cells were plated on poly- d-lysine 24 h prior to transduction. The cells were then treated with either GFP control virus or α9 viruses for 15 h in the presence of polybrene (2 µg/ml; Sigma). The medium was then changed and replaced by fresh RPE medium (Dulbecco’s Modified Eagle’s Medium: F12-10% foetal calf serum-1% penicillin–streptomycin–fungizone).
The cells were kept in culture for 72 h and the transduction efficiency was assessed by analyzing the number of GFP positive cells to 4′,6-diamidino-2-phenylindole positive nuclei. Migration assay quantification Under phase contrast the maximum distance of migration from the edge of the coverslip was measured and the number of cells per 100 µm 2 at various distances counted. Each experimental condition contained at least three coverslips, and each experiment was repeated at least three times using independent samples. Adhesion assay quantification Under phase or epifluorescence random 500 µm square fields were counted. Counts were normalized to control non-coated coverslips. Experiments were repeated at least three times using independent samples. Each experiment contained at least three repeats/coverslips of the same condition.
Cells in 20 random fields were counted in each coverslip. For morphological analysis cells with flat morphology were compared to the control group. Quantification of immunostaining In ImageJ software, cells were selected as areas of interest, then the integrated pixel density of cells in each group standardized to the surface area of the cell and the background signal intensity was subtracted. Statistical analysis Each experiment was repeated at least three times using independent samples and average was calculated.
Each experiment contained at least three repeats/coverslips of the same condition. Cells in 20 random fields were counted in each coverslip in adhesion assays. Inverted coverslip migration assays involving two groups.
The maximum distance of migration was compared between the test and the control group. In addition, the number of cells migrating from the edge of the coverslip was compared with that of the control at the same distance.
Students- t test (two-tailed) was carried out to assess the level of significance. Significance value were represented as. P collagen IV laminin collagen I non-coated, in agreement with previous studies (Ho and Del Priore, ). We treated the cultures with either Mn 2+ or TS2/16 to find out whether increased integrin activation increased the adhesion of RPE cells to these substrates. As shown in, we found that integrin activation by either Mn 2+ or the antibody increased adhesion to all the substrates. RPE cells produce laminin, and therefore over time deposit their own extracellular matrix substrate.
This may explain why addition of Mn 2+ and TS/16 consistently produced a small increase in adhesion of the cells to tissue culture plastic ( ). Effect of integrin activation on RPE cell adhesion to extracellular matrix molecules. Integrin activation with Mn 2+ (500 µM) and TS2/16 antibody increases RPE adhesion to laminin ( A), fibronectin ( B), collagen I ( C) and collagen IV ( D). Extracellular matrix molecules support the adhesion of RPE cells in the order of fibronectin collagen IV laminin collagen I non-coated. All values are normalized to control adhesion (non-coated glass). (ANOVA test:.
P. Effect of integrin activation on RPE cell adhesion to extracellular matrix molecules.
Integrin activation with Mn 2+ (500 µM) and TS2/16 antibody increases RPE adhesion to laminin ( A), fibronectin ( B), collagen I ( C) and collagen IV ( D). Extracellular matrix molecules support the adhesion of RPE cells in the order of fibronectin collagen IV laminin collagen I non-coated. All values are normalized to control adhesion (non-coated glass). (ANOVA test:. P. Effect of integrin activation on RPE cell migration on extracellular matrix molecules. ( A) Integrin activation with Mn 2+ (500 µM) significantly increases maximum distance of migration of RPE cells on all the substrates tested.
Integrin activation significantly increases the number of cells migrating from the edge of coverslip compared to control cells on laminin ( B), fibronectin ( C), collagen I ( D) and collagen IV ( E). N = 3 ( t-test:. P. Effect of integrin activation on RPE cell migration on extracellular matrix molecules.
( A) Integrin activation with Mn 2+ (500 µM) significantly increases maximum distance of migration of RPE cells on all the substrates tested. Integrin activation significantly increases the number of cells migrating from the edge of coverslip compared to control cells on laminin ( B), fibronectin ( C), collagen I ( D) and collagen IV ( E). N = 3 ( t-test:. P. Confirmation of integrin activation by Mn 2+. RPE cells plated on laminin (1 µg/ml) in the absence ( A) and presence ( B) of Mn 2+.
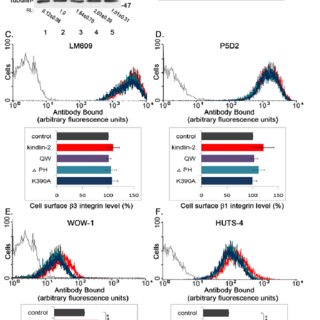
9EG7 binding to β1 integrin is increased following Mn 2+ treatment. Immunostaining for phosphorylated focal adhesion kinase (pFAK) in RPE cells in the absence ( C and E) and presence ( D and F) of Mn 2+ after 1 h and 24 h. ( G and H) Quantification of phosphofocal adhesion kinase levels in RPE cells after Mn 2+ treatment. All values normalized to the levels in the absence of Mn 2+. No difference in total focal adhesion kinase levels ( I) and surface β1 integrin levels ( J) were observed following Mn 2+ treatment. Scale bar = 75 µm.
Confirmation of integrin activation by Mn 2+. RPE cells plated on laminin (1 µg/ml) in the absence ( A) and presence ( B) of Mn 2+. 9EG7 binding to β1 integrin is increased following Mn 2+ treatment.
Immunostaining for phosphorylated focal adhesion kinase (pFAK) in RPE cells in the absence ( C and E) and presence ( D and F) of Mn 2+ after 1 h and 24 h. ( G and H) Quantification of phosphofocal adhesion kinase levels in RPE cells after Mn 2+ treatment. All values normalized to the levels in the absence of Mn 2+. No difference in total focal adhesion kinase levels ( I) and surface β1 integrin levels ( J) were observed following Mn 2+ treatment. Scale bar = 75 µm. Integrin activation increases retinal pigment epithelial cell adhesion and migration on normal Bruch’s membrane Rat intact Bruch’s membrane model Having shown that RPE cell behaviour is changed by integrin manipulation, we needed to see whether these modified behaviours were also seen on Bruch’s membrane. For these experiments, we developed a new model for assessment of RPE cell interactions with intact normal Bruch’s membrane.
Squares of RPE–Bruch’s–choroid–sclera complex were dissected from normal young adult rat eyes. In order to study RPE cell adhesion and migration, the endogenous RPE cells must be removed, which was achieved with water lysis followed by forceful flushing with a pipette, as used in previous studies of glia extracellular matrix biology (Smith-Thomas et al.,; Fidler et al., ) To demonstrate that endogenous RPE cells were removed by this method, treated membranes were cryo-sectioned and stained for two specific RPE markers; RPE-65 and cytokeratin18. This showed that the RPE layer was removed by water treatment but not by incubation in isotonic HBSS. Serial sections at 30 µm intervals were analysed through the whole eye to demonstrate that the water treatment removed RPE cells efficiently ( ).
To demonstrate that this RPE removal method does not damage the underlying basal lamina of Bruch’s membrane, water treated specimens were stained for laminin, revealing that the prominent laminin-positive basement membrane was intact in both water treated and HBSS-treated samples. Scanning electron microscopy of the eyecups showed that untreated or HBSS-treated eyes have an intact continuous layer of regular cobblestone-like RPE cells. After water treatment none of these cells were seen, but instead there was a smooth exposed Bruch’s membrane. Rat Bruch’s membrane preparation and confirmation of RPE layer removal.
Immunostaining for RPE-65, demonstrating the presence of the RPE layer in control HBSS-treated sample ( A) and its absence in a water treated sample ( B). ( C and D) Immunostaining for cytokeratin 18 demonstrating efficient removal of the RPE layer after water treatment. Immunostaining for laminin and cytokeratin 18 shows the presence of intact laminin rich basement membrane in both control treated ( E) and water treated samples ( F). Scale bar = 250 µm. ( G) Staining negative control for RPE-65 and cytokeratin 18. Scanning electron micrographs of the subretinal surface in HBSS control treated ( H) and water treated ( I) samples. Water treatment leads to complete removal of the hexagonal shaped RPE cell monolayer exposing the smooth Bruch’s membrane underneath.
Scale bar = 200 µm. High magnification scanning electron micrographs of HBSS control treated ( J) and water treated ( K) samples. Scale bar = 50 µm. Rat Bruch’s membrane preparation and confirmation of RPE layer removal. Immunostaining for RPE-65, demonstrating the presence of the RPE layer in control HBSS-treated sample ( A) and its absence in a water treated sample ( B).
( C and D) Immunostaining for cytokeratin 18 demonstrating efficient removal of the RPE layer after water treatment. Immunostaining for laminin and cytokeratin 18 shows the presence of intact laminin rich basement membrane in both control treated ( E) and water treated samples ( F). Scale bar = 250 µm.
( G) Staining negative control for RPE-65 and cytokeratin 18. Scanning electron micrographs of the subretinal surface in HBSS control treated ( H) and water treated ( I) samples. Water treatment leads to complete removal of the hexagonal shaped RPE cell monolayer exposing the smooth Bruch’s membrane underneath. Scale bar = 200 µm. High magnification scanning electron micrographs of HBSS control treated ( J) and water treated ( K) samples. Scale bar = 50 µm. Integrin activation increases retinal pigment epithelial cell adhesion and migration on Bruch’s membrane Using the same adhesion and migration assays described above, RPE behaviour on Bruch’s membrane was assessed.
To do this, squares of RPE-free Bruch’s membrane were stuck to the bottom of the chamber slide wells. ARPE-19 cells were labelled using vibrant Di-I, which labelled 99% of the cells allowing them to be visualized by fluorescence microscopy. To explore the role of integrin activation in RPE adhesion to the intact Bruch’s membrane, adhesion assays were carried out in the presence of Mn 2+ and TS2/16. The number of cells attached and the percentage of cells with flat morphology were analysed after 1 h. Both Mn 2+ and TS2/16 increased the number of RPE cells attached to the Bruch’s membrane, and greatly increased the percentage of cells that had spread out with a flat morphology (A). RPE migration on Bruch’s membrane was assessed using the inverted coverslip assay, performed in the presence of a mitotic inhibitor to eliminate the effects of cell proliferation. Integrin activation increased the maximum distance of migration and the number of cells migrating from the edge of coverslip compared to the control samples (B).
These results suggest that increasing integrin activation can increase the interaction of RPE cells with the extracellular matrix molecules in Bruch’s membrane, enhancing the adhesion and migration of the cells. Effect of integrin activation on RPE adhesion and migration on rat Bruch’s membrane. ( A) Mn 2+ and TS2/16 application both increase the number of cells attached and the percentage of cells with flat morphology on Bruch’s membrane.
White arrows point to examples of cells with flat morphology in each group. N = 3 (ANOVA:. P. Effect of integrin activation on RPE adhesion and migration on rat Bruch’s membrane. ( A) Mn 2+ and TS2/16 application both increase the number of cells attached and the percentage of cells with flat morphology on Bruch’s membrane. White arrows point to examples of cells with flat morphology in each group. N = 3 (ANOVA:.
P. Effect of integrin activation on RPE adhesion on human Bruch’s membrane.
( A) Integrin activation with Mn 2+ and TS2/16 increases RPE adhesion to pathological Bruch’s membrane from wet age-related macular degeneration patients. N = 3 (ANOVA test:.
P. Effect of integrin activation on RPE adhesion on human Bruch’s membrane. ( A) Integrin activation with Mn 2+ and TS2/16 increases RPE adhesion to pathological Bruch’s membrane from wet age-related macular degeneration patients. N = 3 (ANOVA test:.
P. Effect of TN-C on RPE cell adhesion and migration. ( A) TN-C inhibits RPE cell adhesion in a dose responsive manner. Maximal inhibition is achieved at 10 µg/ml of TN-C. Control corresponds to adhesion on non-coated glass coverslips. Effect of TN-C on RPE cell adhesion and migration. ( A) TN-C inhibits RPE cell adhesion in a dose responsive manner.
Maximal inhibition is achieved at 10 µg/ml of TN-C. Control corresponds to adhesion on non-coated glass coverslips. Effect of integrin activation on RPE cell behaviour on TN-C. ( A) Integrin activation by application of Mn 2+ enabled RPE cells to adhere to a TN-C coated surface.
Non-coated glass coverslip was used for the control. N = 3, ANOVA:. P. Effect of integrin activation on RPE cell behaviour on TN-C. ( A) Integrin activation by application of Mn 2+ enabled RPE cells to adhere to a TN-C coated surface. Non-coated glass coverslip was used for the control.
N = 3, ANOVA:. P. Effect of α9 integrin expression on RPE cell adhesion and migration on TN-C.
( A) Alpha9 expression increases RPE cell adhesion compared to GFP-expressing control RPE cells. Adhesion levels normalized to control GFP cells.
N = 3 ( t-test. P. Effect of α9 integrin expression on RPE cell adhesion and migration on TN-C. ( A) Alpha9 expression increases RPE cell adhesion compared to GFP-expressing control RPE cells.
Adhesion levels normalized to control GFP cells. N = 3 ( t-test. P.
Effect of α9 integrin expression on RPE cell adhesion to human Bruch’s membrane. Immunostaining for TN-C on Bruch’s membranes derived from patients with wet age-related macular degeneration (AMD) ( A) and control subjects ( B). Both submacular (Submac) and peripheral (Peri) areas in wet age-related macular degeneration show raised TN-C levels compared to similar areas in the control non-age-related macular degeneration membranes. Scale bar = 100 µm. ( C) Integrin α9 expression increases RPE cell adhesion to wet-age-related macular degeneration membranes while having no effect on control membranes. N = 3 (ANOVA:. P.
Effect of α9 integrin expression on RPE cell adhesion to human Bruch’s membrane. Immunostaining for TN-C on Bruch’s membranes derived from patients with wet age-related macular degeneration (AMD) ( A) and control subjects ( B). Both submacular (Submac) and peripheral (Peri) areas in wet age-related macular degeneration show raised TN-C levels compared to similar areas in the control non-age-related macular degeneration membranes. Scale bar = 100 µm. ( C) Integrin α9 expression increases RPE cell adhesion to wet-age-related macular degeneration membranes while having no effect on control membranes. N = 3 (ANOVA:.
P.
